If you have a tooth that’s badly decayed, you might worry that losing it is the only option. The good news is that root canals can often save severely decayed teeth by removing infection and protecting your natural tooth.
This treatment helps relieve pain and stops decay from spreading. It gives you a chance to keep your own smile.
Knowing when to consider a root canal is important. You might notice signs like sharp pain, sensitivity, or swelling that signal the inside of your tooth is infected.
Understanding what happens during the root canal process can ease your worries. It can help you make the best choice for your dental health.
Key Takeaways
- Root canals can save teeth that are severely decayed.
- Early symptoms can help you know when to see your dentist.
- Taking care of your tooth after treatment helps it last longer.
Experiencing Tooth Pain in Wilmington?
Can Root Canals Save Severely Decayed Teeth?
If your tooth is badly damaged or infected, there is a chance you can save it instead of having it pulled. Root canals focus on removing infection deep inside the tooth and protecting the natural tooth structure.
This gives you relief while keeping your smile intact.
How Root Canals Work to Save Damaged Teeth
A root canal treatment removes the infected soft tissue inside your tooth, called the pulp. This pulp contains nerves and blood vessels, so when it’s infected, you often feel pain or sensitivity.
During the procedure, the dentist cleans out the infected material from the tooth’s inner chambers. Then, they fill and seal these spaces with a safe material to stop bacteria from returning.
Finally, the tooth is restored with a crown or filling to strengthen it. This helps your tooth stay in place and work properly while preventing further damage.
Root canal treatments have a success rate of over 95% when properly performed and restored.
When Is a Tooth Too Decayed for a Root Canal?
Sometimes, a tooth may be too damaged for a root canal to help. If the decay has destroyed most of the tooth structure or if there is a severe crack that can’t be fixed, extraction might be the only option.
Your dentist will take X-rays and examine the tooth carefully to decide this. If there’s a large abscess or the infection has spread beyond repair, saving the tooth may not be possible.
However, many severely decayed teeth can still be treated with root canal therapy if the infection hasn’t caused too much structural damage.
Tooth Structure and Eligibility for Root Canal Therapy
Your tooth has multiple layers: enamel on the outside, dentin beneath it, and the soft pulp inside. Root canals become necessary when decay passes through the enamel and dentin to reach the pulp.
For the treatment to work, enough healthy tooth structure must remain after cleaning out the decay. This allows the tooth to be sealed and restored properly.
If the outer layers are intact enough for a crown or filling after treatment, root canal therapy is usually a good fit. This helps you keep your natural tooth and avoid gaps that affect chewing and jaw health.
Book a Root Canal Evaluation in Wilmington Today
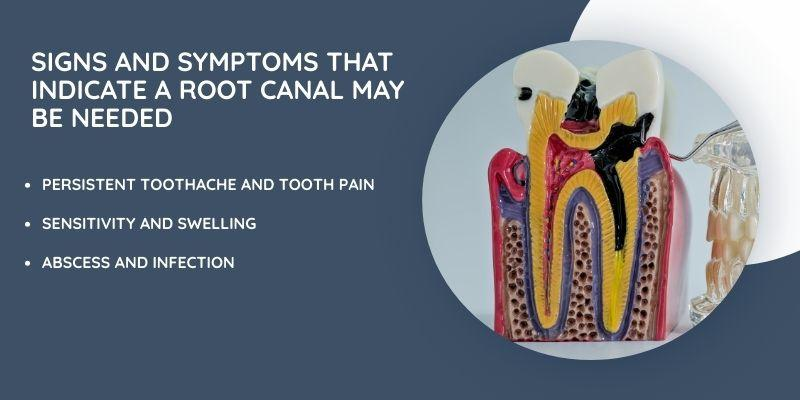
Signs and Symptoms That Indicate a Root Canal May Be Needed
When your tooth starts causing trouble, it’s important to watch for specific signs that point to a serious problem inside. These signs can include pain that sticks around, strange feelings when you eat or drink, or swelling around the tooth.
Knowing these early can help you get the right care before things get worse.
Persistent Toothache and Tooth Pain
If you have a toothache that just won’t quit, it’s a strong sign you might need a root canal. The pain can feel deep in the bone of your tooth or even spread to your jaw, face, or other teeth.
Sometimes the pain comes and goes, but it usually comes back. Tooth pain like this is often caused by infections or damage to the tooth’s nerves and pulp, which is the soft tissue inside your tooth.
If tooth decay reaches this pulp, it can cause lasting discomfort. Other issues can also cause tooth pain, but when the ache lasts a long time or gets worse, it’s a smart move to see your dentist.
Dealing with pain early can save your tooth and avoid bigger problems.
Sensitivity and Swelling
When eating hot or cold food makes your tooth hurt, it could mean the nerves inside are damaged or infected. This sensitivity might feel like a sharp pain or a dull ache.
Usually, if the pain stays even after you stop eating or drinking, it’s a warning sign. Swelling near your tooth can also show that there’s an infection.
Your gums might puff up, feel tender, or sometimes have a small bump called a gum boil. This happens because dead tissue inside the tooth releases waste that irritates the area around it.
Swelling can come and go, but it means your body is fighting an infection that needs attention before things get worse.
Abscess and Infection
An abscess is a serious sign that the infection has spread beyond the tooth pulp to the surrounding bone and gums. This often causes a painful swelling or a small pimple on your gum that might leak pus.
The infection can lead to bad taste in your mouth and bad breath. It can also make your tooth feel loose because the bone around the root is getting weaker from the infection.
If you notice any swelling, a bad smell, or a painful bump, it’s important to see your dentist quickly. A root canal can clean out the infection and save your tooth before the damage spreads further.
You can learn more about these symptoms and when to act on them at signs you might need a root canal.
Don’t Lose Your Tooth; Explore Root Canal Treatment
Root Canal Procedure: What to Expect
The root canal process is done carefully to remove infection while saving your natural tooth. It involves getting your tooth ready, cleaning out the damaged tissue, and then sealing and restoring the tooth to protect it.
Preparing for the Dental Procedure
Before the root canal starts, your dentist will take X-rays to see the damage and plan the treatment. You’ll get a local anesthetic to numb the area around the infected tooth.
This helps make the procedure comfortable and pain-free. Once the area is numb, the dentist will place a small barrier called a dental dam.
This keeps your tooth dry and free from saliva during the treatment. You might feel some pressure, but you shouldn’t feel sharp pain.
Preparing this way helps your dentist work carefully and keeps the procedure clean.
Removal of Infected Pulp and Cleaning the Tooth
Next, the dentist makes a small hole in the crown of your tooth to reach the infected pulp inside. Using special tools, they remove the infected tissue and dead nerves from the root canals.
This step is important because the infected pulp can cause ongoing pain and infection if not removed. Afterward, the canals are cleaned thoroughly with antiseptic solutions to kill any remaining bacteria.
Your dentist will shape the canals to make sure they can be sealed properly later. This cleaning helps prevent future infections and protects your tooth structure.
Sealing and Restoring the Tooth
Once the canals are clean and dry, your dentist fills them with a rubber-like material called gutta-percha. This seals the canals and keeps bacteria from getting inside.
A temporary or permanent filling is placed on top to close the hole made earlier. In many cases, your dentist will recommend a crown to cover the tooth.
Crowns protect the tooth from breaking and restore its strength and function. This final step helps you keep your natural tooth for many years while supporting normal chewing and preventing further damage.
Comparing Root Canals and Tooth Extractions
When a tooth is severely decayed or infected, you face a choice between saving it or removing it. Both options have pros and cons, and understanding them can help you protect your smile and oral health.
Benefits of Saving the Natural Tooth
Keeping your natural tooth with a root canal helps maintain your bite and jaw structure. The procedure removes infected pulp but leaves the main tooth intact.
This keeps nearby teeth from shifting, which can happen after tooth loss. A root canal also preserves chewing function, so you won’t have to change how or what you eat.
Teeth treated with root canal therapy and crowns can last 10–20 years or longer.
Plus, saving your tooth avoids costly replacements like implants or bridges. Recovery from a root canal is usually quick, with only mild discomfort.
You’ll likely get a crown afterward to protect the tooth, making it strong and natural-looking.
When Extraction Is Unavoidable
Sometimes, your tooth may be too damaged to save. If the decay or infection has severely weakened it, extraction becomes necessary to stop pain and prevent spread.
Extraction removes the problem tooth completely. While it ends infection risk in that tooth, losing it can cause other issues.
Nearby teeth may shift, and jawbone loss over time can affect your facial structure. After extraction, you’ll often need a replacement like an implant, bridge, or denture to restore chewing and appearance.
These replacements add cost and require extra care to maintain. In cases like overcrowding or impacted teeth, extraction may also protect your overall oral health.
Your dentist will help decide if it’s the right choice for you.
Learn more about the advantages and impacts of these choices at premieredental.com/root-canal-vs-tooth-extraction.
Root Canal Retreatment and Long-Term Outcomes
Root canal therapy can often save a severely damaged tooth, but sometimes the treatment may need to be redone. Understanding why retreatment happens and what it involves can help you make informed choices about your oral health.
Why Retreatment May Become Necessary
Even a successful root canal may fail years later. This can happen if bacteria re-enter the tooth or if the original filling doesn’t fully seal the canals.
Other reasons include new decay, cracks, or damage that lets infection back in. Symptoms like pain, swelling, or sensitivity can signal the need for retreatment.
Sometimes, there are no clear symptoms, but X-rays show problems. Ignoring these signs can lead to more serious dental issues or tooth loss.
Retreatment gives your tooth a second chance by addressing problems that the first treatment missed or that developed afterward. It’s a way to keep your natural tooth without having to extract and replace it.
What Happens During Root Canal Retreatment
The dentist first removes the old filling material from your tooth’s canals. Then, they clean out the infection carefully using special tools.
This step removes bacteria and damaged tissue to help your tooth heal. Next, the dentist shapes and fills the canals again to create a tight seal.
This step helps prevent new infection. Finally, your tooth will be restored with a crown or filling to protect it.
Retreatment may take one or more visits depending on how complex the problem is. Your dentist will also check for cracks or other issues that might affect the long-term success of the treatment.
Oral Hygiene Tips After a Root Canal
Taking care of your tooth after a root canal is important to keep it healthy and prevent problems. This means keeping your mouth clean and protecting the treated tooth from new issues.
Simple habits can help you heal well and avoid future tooth decay.
Maintaining Oral Health Post-Treatment
After your root canal, gentle but thorough cleaning is key. Brush your teeth twice a day with a soft-bristled toothbrush.
Be careful around the treated tooth to avoid irritation. Use fluoride toothpaste to help strengthen your tooth enamel.
Floss daily, but avoid the treated area if it feels sensitive. Rinsing your mouth with warm salt water can reduce swelling and fight bacteria.
Remember to follow any instructions from your dentist about medication or special cleaning tips. Keeping the treated area clean lowers the risk of infection and helps you heal faster.
Regular dental checkups let your dentist monitor your tooth’s health and catch problems early.
Preventing Future Tooth Decay
Protecting your teeth after a root canal means more than just caring for the treated tooth. You should avoid sugary and sticky foods that can cause cavities elsewhere in your mouth.
Eating soft, cool, and nutritious foods helps avoid irritation to the root canal site. Drink plenty of water and cut back on acidic drinks that wear down enamel.
If you smoke or use tobacco, try to quit, because these habits increase the chance of gum disease and tooth decay. Using a mouthguard when you play sports or grind your teeth protects all your teeth from damage.
Learn more about keeping your teeth strong and clean after treatment from detailed oral hygiene tips.
Frequently Asked Questions
You might wonder about what happens after the procedure, how much it costs, or how you can avoid needing one in the future. There are also questions about the tools and medicines used, how your tooth will look, and how root canals differ from regular fillings.
Here are clear answers to help you understand these details.
What are the potential side effects after a root canal treatment?
After a root canal, you may experience some sensitivity or mild pain around the treated tooth. This usually lasts a few days and can be controlled with over-the-counter pain relievers.
In some cases, swelling or discomfort may occur, but this often gets better with time. If pain or swelling gets worse, you should contact your dentist.
How much does a typical root canal procedure cost?
The cost varies based on the tooth’s location and how complex the treatment is. On average, front teeth are less expensive to treat than molars.
Costs may range from a few hundred to over a thousand dollars. Your insurance might cover part of the expense, so check with your provider before treatment.
Are there effective ways to prevent needing a root canal?
You can greatly reduce your risk by brushing twice each day with fluoride toothpaste and flossing daily. Avoiding sugary foods and drinks also helps prevent decay.
Regular dental checkups let your dentist find problems early, which means less chance of infection spreading to the pulp of your teeth.
What medications are used inside the tooth during a root canal?
Dentists use special disinfectant solutions to clean out bacteria and infected tissue inside the tooth. They also place medicated dressings or fillers that help stop infection and promote healing.
After cleaning, a biocompatible material fills the empty space to seal the tooth and stop new bacteria from entering.
What can I expect to see in my tooth’s appearance before and after a root canal?
Before treatment, your tooth might be darkened, chipped, or swollen at the gums. You could also have visible cracks or decay.
After the procedure, the tooth is cleaned and sealed. Often, a crown is placed on top to restore its look and strength, making it look and work like a natural tooth again.
How does a root canal treatment differ from filling a cavity?
A filling treats decay that only affects the outer part of your tooth, called the enamel or dentin. It cleans out decay and fills the space.
A root canal goes deeper, targeting infected or damaged pulp inside the tooth. It removes nerve tissue and infection, then seals the inside.
Often, a crown is needed for extra protection after a root canal. Root canals are used when decay or damage reaches the tooth’s center.
Fillings are for less severe problems.