You want full mouth dental implants, but you may wonder if your jawbone can support them. When teeth have been missing for a while, bone loss often follows. Gum disease, injury, or long-term denture use can also weaken the bone.
You need bone grafting for full mouth dental implants when your jaw does not have enough healthy bone to hold the implants in place.
Implants must fuse with strong bone to stay stable. If your bone is too thin or soft, a graft can rebuild the area and create a solid base.
You have options, and modern techniques can often restore lost bone or even avoid grafting in some cases.
Understanding when full mouth dental implants bone grafting become necessary helps you plan your treatment with confidence and know what to expect before you start.
Key Takeaways
- Full mouth implants require enough healthy jawbone for long-term stability.
- Bone grafting rebuilds areas where bone loss has occurred.
- Some implant techniques may reduce or avoid the need for grafting.
Understanding Full Mouth Dental Implants and Jawbone Health
Full mouth dental implants replace all or most of your teeth with fixed restorations that anchor into your jawbone. Your bone health directly affects how stable, strong, and long‑lasting your implants will be.
What Are Full Mouth Dental Implants
Full mouth dental implants replace all teeth in your upper jaw, lower jaw, or both. Instead of placing one implant for each missing tooth, your dentist places a set number of dental implants to support a full arch of teeth.
Common systems include All-on-4, All-on-6, and All-on-8. These methods use four to eight implants per arch to hold a fixed bridge.
Each implant is a small titanium post placed into your jawbone. After healing, your dentist attaches a custom prosthetic that looks and functions like natural teeth.
Unlike dentures, these teeth stay in place. You do not remove them at night, and they do not rely on adhesives.
Role of the Jawbone in Implant Success
Your jawbone acts as the foundation for dental implants. Without enough bone height and density, the implant cannot anchor securely.
When you lose teeth, your jawbone begins to shrink. This process is called bone resorption. Over time, the bone loses volume because it no longer receives stimulation from tooth roots.
Full mouth dental implants help slow this process. Implants stimulate the jawbone during chewing, which helps maintain bone structure.
If your bone has already thinned, your dentist may recommend bone grafting. A graft rebuilds volume so your implants have enough support.
Osseointegration and Implant Stability
Osseointegration is the process by which your jawbone grows around and bonds to the implant surface. This step determines whether your dental implants stay stable over time.
After placement, your implant needs several months to fuse with the bone. During this period, new bone cells attach directly to the titanium post. When fusion completes, the implant becomes part of your jaw structure.
Strong osseointegration allows you to bite and chew with confidence. Weak bonding can lead to movement, discomfort, or implant failure.
Your bone quality, overall health, and oral hygiene all affect this process. Healthy bones and good care improve long‑term implant stability and help protect your full mouth dental implants for years.
Schedule an appointment in Hampstead, NC, to see if you need bone grafting for full mouth implants.
When Bone Grafting Is Necessary for Dental Implants
Full mouth dental implants need strong, stable bone to stay secure. If your jaw has shrunk or weakened, bone grafting may rebuild the support required for safe implant placement.
Common Causes of Jawbone Loss
Jawbone loss often starts after you lose a tooth. When the tooth root no longer stimulates the bone, bone resorption begins. Your body slowly absorbs the unused bone, which reduces height and width.
Gum disease also plays a major role. Infection can destroy the bone that supports your teeth, sometimes without clear pain at first.
Injury, past dental infections, or long-term denture use can also thin the jaw. Dentures do not replace tooth roots, so they do not stop bone shrinkage.
Many implant patients need grafting because of these changes.
A dental bone graft adds volume where bone has worn away. This rebuilds the base needed for full arch restorations.
How Bone Density Affects Implant Placement
Implants must fuse with your jaw in a process called osseointegration. This fusion depends on strong bone density.
If your bone is too soft or too thin, the implant may not anchor well. Poor density can lead to movement during healing, which raises the risk of failure.
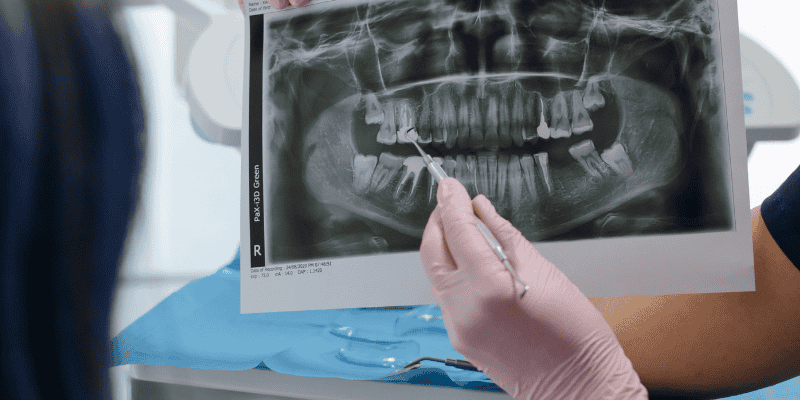
Your dentist checks bone quality before implant placement. They often use a CBCT scan, also known as cone beam computed tomography, to measure bone height, width, and density in three dimensions.
These scans show the exact problem areas. If they reveal weak spots, bone grafting can strengthen the site before implants go in. Strong bone helps your implants handle daily chewing forces without shifting.
Signs You Might Need a Bone Graft
You may not feel bone loss, but certain signs raise concern. Long gaps after tooth loss often mean the jaw has shrunk.
Loose dentures can also signal ongoing bone resorption. If your dentures no longer fit well, your ridge may have become thinner.
Your dentist may see warning signs on imaging tests. A CBCT scan can show low bone height in the upper jaw or narrow ridges in the lower jaw.
Common clinical findings include:
- Thin jaw ridge
- Low sinus floor in the upper jaw
- History of advanced gum disease
- Old tooth extractions without replacement
If these issues appear, grafting creates the support needed for stable implants. Planning ahead lowers the chance of complications during surgery.
Alternatives to Bone Grafting
Some patients qualify for alternatives to bone grafting. Your dentist decides this based on your bone shape and health.
Short implants can work when bone height is limited but still strong. These implants require less depth.
Angled implants may avoid thin areas of bone. In severe upper jaw loss, providers may suggest specialized options like zygomatic implants.
Not everyone needs a graft. Careful imaging and planning help you choose the safest and most predictable path for full mouth implant treatment.
Types of Bone Graft Procedures and Materials
Bone grafting rebuilds areas of your jaw that lack enough bone to hold full mouth implants. The right procedure and bone graft material depend on how much bone you have lost and where the implants will go.
Overview of Grafting Procedures
Your dentist chooses a grafting method based on the size and location of bone loss. Some procedures add a small amount of bone, while others rebuild large sections of the jaw.
Common dental bone grafting procedures include:
- Socket preservation: Placed right after a tooth is removed to prevent bone shrinkage.
- Ridge augmentation: Rebuilds the width or height of the jawbone.
- Sinus lift: Adds bone under the sinus when upper back teeth need implants.
A dental bone graft increases jawbone volume by placing natural or lab-made material in areas with bone loss. Over time, your body replaces or blends this material with your own bone.
Healing may take a few months. Larger grafts often need more time before you can place full mouth dental implants.
Types of Bone Grafts
Dentists use several types of bone grafts, each with clear benefits and limits. The best choice depends on your health, the size of the defect, and how fast you need results.
| Type | Source | Key Point |
| Autograft | Your own bone | Strong bone growth requires a second surgical site |
| Allograft | Donor human bone | No second surgery, widely used |
| Xenograft | Animal bone, often bovine | Acts as a scaffold for new bone |
| Alloplast | Synthetic material | No human or animal tissue used |
Your dentist may also combine graft types to improve stability and healing.
Choosing Bone Graft Materials
You have several types of bone graft materials, and each works in a specific way. Some stimulate new bone growth, while others act as a framework that your bone grows into.
Common bone substitute materials include:
- Hydroxyapatite: A mineral similar to natural bone.
- Bioactive glass: Bonds with bone and supports healing.
- Alloplast materials: Synthetic options used when you prefer no donor tissue.
Your dentist looks at bone thickness, implant position, and your medical history before choosing a bone graft material. If you smoke or have certain health conditions, healing may take longer.
The goal is simple: create a stable base so your full mouth implants can stay secure for years.
Request a consultation to find out if bone grafting is needed before implants.
Key Bone Grafting Techniques for Full Mouth Implants
When you plan for full mouth dental implants, your dentist may need to rebuild areas of weak or thin jawbone. The right bone graft procedure creates stable support so your implant surgery can succeed.
Sinus Lift and Sinus Augmentation
If you need implants in your upper back jaw, you may not have enough bone height under your sinus. A sinus lift, also called sinus augmentation, adds bone between your upper jaw and the sinus cavity.
During this bone graft procedure, your surgeon gently lifts the sinus membrane. They place graft material in the space to increase bone height.
Over several months, your body replaces the graft with new bone through natural bone regeneration.
You may need this treatment if you lost upper molars years ago. Bone shrinks over time, and the sinus expands into that space.
Healing often takes 4 to 9 months before implants can be placed, depending on your case.
Ridge Augmentation for Jawbone Width or Height
If your jaw is too thin or too short, your dentist may recommend ridge augmentation. This method rebuilds the shape and size of your jaw so it can hold implants securely.
Surgeons place bone graft material along the ridge of your jaw. In some cases, they use a small block of your own bone and secure it with tiny screws. In others, they use donor or synthetic material.
You may need ridge augmentation if you have:
- Long-term tooth loss
- Advanced gum disease
- Bone damage from injury
This treatment increases jaw width or height, which helps your implants stay stable under daily chewing pressure. Healing usually takes several months, but it gives your full arch implants a stronger base.
Minor Bone Grafting Procedures
Not all cases require large grafts. You may only need minor bone grafting if your bone loss is small and limited to certain areas.
Common minor procedures include:
- Socket preservation after tooth removal
- Small grafts around implant sites
- Guided bone regeneration with a protective membrane
These treatments support bone regeneration in focused spots. For example, placing graft material right after a tooth extraction helps prevent the ridge from shrinking.
Minor grafts often heal faster than large ridge procedures and may allow implant surgery within a few months, depending on your healing and overall health.
Bone Grafting Process: From Consultation to Recovery
You move through clear steps, from imaging and planning to surgery and healing. Each phase affects how well your implants bond with your jaw and how long your results last.
Evaluating Candidacy With Imaging and Consultation
Your dental implant consultation sets the plan in motion. The dentist or oral surgeon reviews your health history, medications, and any past gum disease.
They take digital X-rays and often a 3D CBCT scan. These images show bone height, width, and density in each part of your jaw.
If large areas of bone have shrunk, you may need grafting before full mouth dental implants. If bone loss is mild, the surgeon may place a small graft at the same time as the implant.
During this visit, you also discuss timing and cost. Some cases need tooth removal first, which can extend treatment. If you need grafting before implants, it can add 2 to 6 months to your timeline.
You leave this visit with a clear treatment plan and a schedule for surgery and follow-up appointments.
Bone Graft Surgery and Implant Timing
The bone graft procedure usually takes place in a dental office or surgical suite. Your oral surgeon numbs the area with local anesthesia, and you may choose sedation if you feel anxious.
The surgeon places graft material in the weak area of your jaw. This material can come from your own bone, a donor source, or a synthetic option. The goal is to create a stable base for implants.
After placement, the surgeon closes the gum tissue with stitches. Over time, your body replaces the graft material with natural bone.
Healing time depends on the size of the graft. Initial recovery takes about a week, but the graft itself needs at least three months to heal. Larger grafts may take up to nine to 12 months, as explained in this guide on dental bone graft recovery and healing time.
Your surgeon schedules implant placement once imaging shows solid new bone.
Bone Graft Recovery and Aftercare
Bone graft recovery starts right after surgery. You can expect swelling, tenderness, and mild bruising for several days.
You manage discomfort with prescribed or over-the-counter pain medicine. Your provider may also give you antibiotics to lower the risk of infection.
Follow these basic aftercare steps:
- Eat soft foods for several days.
- Avoid smoking or vaping, which slows healing.
- Do not disturb the surgical site with your tongue or fingers.
- Skip heavy lifting and hard exercise for at least 48 hours.
You might notice tiny bone particles that look like grains of sand. Small amounts are normal in the first few days.
You attend follow-up appointments so your dentist can check healing and remove stitches if needed. Imaging later confirms that the graft has fused with your natural bone.
Potential Risks and How to Avoid Graft Failure
Most bone graft procedures heal without problems. Still, graft failure can happen if the new bone does not bond well with your jaw.
Common risk factors include:
- Smoking
- Poor oral hygiene
- Uncontrolled diabetes
- Active gum infection
Infection at the surgical site can also cause graft failure. Signs include severe pain, swelling that gets worse, pus, or fever. You should call your oral surgeon right away if these occur.
You reduce your risk by following all aftercare instructions and keeping your follow-up appointments. Brush gently, keep the area clean, and take all medications as directed.
When you protect the graft during healing, you give your future full mouth dental implants the strong base they need.
All-on-4 Implants and Graftless Solutions
All-on-4 offers a way to replace a full arch of teeth with fewer implants and, in many cases, no bone grafting. You get a fixed set of teeth that attaches to four implants placed in strong areas of your jaw.
What Makes All-on-4 Different
Traditional full mouth dental implants often use six to ten implants per arch. All-on-4 uses four implants per arch, placed in specific positions to support a full bridge.
Two implants go straight into the front of your jaw. The other two sit at an angle in the back. This angled implant placement lets your surgeon use denser bone and avoid areas like the sinus cavity in the upper jaw.
This approach supports a full arch of 10 to 14 teeth on the same day in many cases. Because the dental bridges attach to implants, it does not rest on your gums like a denture. That design improves stability and function.
When All-on-4 Avoids Bone Grafting
Bone grafting becomes necessary when your jawbone lacks enough height or width to hold implants securely. All-on-4 often reduces that need by using existing bone more efficiently.
The angled back implants anchor into thicker bone toward the front of your jaw. This technique often avoids sinus lifts in the upper jaw and reduces the need for vertical bone grafts.
You may qualify for this graftless option even if you have moderate bone loss. However, severe bone loss can still require grafting. Your surgeon will use scans to measure bone density and decide if you need added support.
Benefits and Limitations of Graftless Options
Benefits of graftless All-on-4:
- Fewer implants placed
- Shorter treatment time
- Lower chance of needing bone graft surgery
- Faster return to daily function
You often leave surgery with a temporarily restored smile. This allows you to speak and eat soft foods while healing.
All-on-4 implants also help stimulate your jawbone. The titanium posts fuse with bone and help maintain structure.
Still, this method has limits. You rely on four implants to support an entire arch. If one fails, it can affect the whole bridge. Not every patient qualifies, especially if bone loss is extreme or if health conditions affect healing.
Your dentist will weigh these factors before recommending graftless restorative dental treatments.
Take the next step toward a secure smile by exploring your bone grafting and implant options today.
Frequently Asked Questions
Bone grafting adds time and cost to full mouth dental implants, but it can improve stability and long-term results. You should understand pricing, healing time, risks, and success rates before you move forward.
What is the typical cost for a dental bone graft procedure?
You can expect the cost to vary based on the size of the graft and the type of material used. Small grafts for one site often cost less than large grafts done for full arch cases.
The total fee depends on the graft material, surgical time, and case complexity, as explained in this guide on dental bone graft procedure costs and risks.
Insurance may cover part of the cost if the graft is medically necessary, but many plans limit coverage.
Your dentist should give you a written treatment plan with exact fees before you schedule surgery.
How long should I wait between a bone graft and placing a dental implant?
You usually wait several months before placing implants. Many patients heal in about 4 to 6 months, but larger grafts can take longer.
The graft needs time to fuse with your natural bone in a process called osseointegration. Your dentist will check healing with exams and imaging before moving forward.
Can you describe the healing stages after a dental bone graft?
In the first few days, you may notice swelling, mild bleeding, and soreness. Pain usually improves within a week.
Over the next few months, your body replaces the graft material with new bone. The graft acts as a scaffold while your bone cells grow into the area.
Your dentist will monitor this growth before placing implants.
What are the signs that a dental bone graft may have failed?
Severe pain that does not improve, ongoing swelling, or signs of infection may point to a problem. Pus, fever, or a bad taste in your mouth also need attention.
You may also notice that small graft particles come out, but this can be normal in minor amounts. Call your dentist right away if symptoms worsen instead of improve.
Is a bone graft necessary for tooth extraction if I’m not planning on getting an implant?
You do not always need a graft after an extraction. However, bone shrinks quickly once a tooth is removed.
If you think you may want implants later, preserving bone now can make future treatment easier. If you plan to use dentures, your dentist may still suggest grafting to help maintain jaw shape.
What’s the usual success rate of dental implants that require bone grafting?
Dental implants placed in grafted bone can succeed at rates similar to implants placed in natural bone when the graft heals well. Success depends on your health, oral hygiene, and the quality of the graft.
Bone grafting helps create a stable base for implants, which improves long-term support. Following your dentist’s care instructions plays a key role in keeping your implants secure.