Many people wonder if they’re too old for dental implants once they reach their 60s, but age alone doesn’t determine whether you can get implants.
Your eligibility for dental implants after 60 depends on your bone quality, gum health, and overall medical condition rather than your age.
In fact, dental implants can last decades or even a lifetime with proper care, making them a worthwhile investment at any age.
Your body does go through changes after 60 that affect how dental implants work. You might have experienced some bone loss in your jaw or have health conditions that need special attention.
The good news is that modern dental technology has solutions for these challenges, and many older adults successfully receive implants that improve their quality of life.
Understanding what to expect can help you make an informed decision about tooth replacement.
This guide covers everything about dental implants for seniors, including what the process involves and how to keep your implants healthy for years to come.
Key Takeaways
- Age itself doesn’t prevent you from getting dental implants if you have adequate bone density and good overall health
- Dental implants help preserve your jawbone and facial structure while restoring your ability to eat and speak properly
- Proper oral hygiene and regular dental visits are essential for maintaining your implants as you age
Why Dental Implants Matter After 60
Dental implants provide fixed tooth replacement that protects jawbone health and restores full chewing ability. Unlike removable options, implants stay secure and feel like natural teeth.
How Dental Implants Benefit Seniors
The benefits of dental implants for seniors go beyond appearance. When you lose teeth, your jawbone begins to shrink because it no longer receives pressure from chewing. This bone loss changes your face shape over time, making you look older.
Dental implants stop this process by acting like natural tooth roots. They transfer chewing force directly into your jawbone, which keeps the bone active and healthy. This means your facial structure stays supported.
You’ll also eat more comfortably. Implants restore about 80-90% of normal chewing strength, letting you enjoy foods that dentures make difficult. Apples, corn on the cob, and steak become possible again.
Speech improves too. Missing teeth or loose dentures can cause slurring or clicking sounds. Fixed implants let you speak clearly without worry.
Comparing Tooth Replacement Options
Your main tooth replacement options include dentures, bridges, and implants. Each works differently.
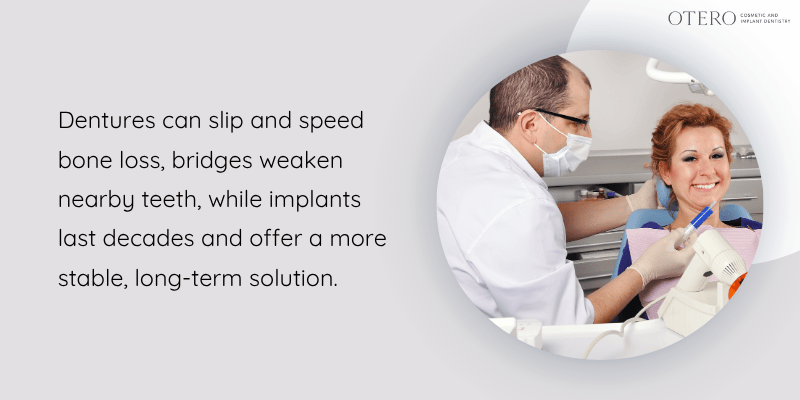
Dentures sit on your gums and need adhesive to stay in place. They slip during eating and speaking. They also speed up bone loss because they don’t stimulate the jawbone. You’ll need replacements every 5-7 years as your jaw shape changes.
Bridges use neighboring teeth as anchors. Your dentist must grind down healthy teeth to attach the bridge. This puts extra stress on those teeth and can damage them over time.
Dental implants don’t affect other teeth. They’re placed directly into your jawbone and can last 25 years or more with proper care.
While they cost more upfront, you won’t need frequent replacements. The initial investment often saves money long-term.
Unique Considerations for Dental Implants in Older Adults
Getting dental implants after 60 requires careful evaluation of your bone health, medical conditions, and medications. These factors play a bigger role in your treatment success than your actual age.
Bone Density and Jaw Health
Your jawbone needs enough density and volume to support dental implants. As you age, your bone naturally loses density, especially if you’ve had missing teeth for several years.
Your dentist will perform a bone density evaluation before placing implants. This usually involves X-rays or CT scans to measure your bone quality. Lower bone density is associated with higher rates of implant failure, so this step is critical.
Conditions like osteomalacia reduce bone mass and can affect osseointegration. This is the process where your implant fuses with your jawbone.
If you have vitamin D deficiency or low calcium levels, your dentist may recommend supplements before surgery.
You might need a bone graft if your jaw lacks sufficient density. This procedure adds bone material to strengthen your jaw before implant placement.
Overall Medical and Oral Health Factors
Your existing health conditions affect how well dental implants work for older adults. Diabetes, cardiovascular disease, and autoimmune conditions require special attention during treatment planning.
Periodontitis increases your risk of peri-implantitis, which is inflammation around the implant. You need healthy gums before getting implants. Your dentist will treat any gum disease first.
If you have rheumatoid arthritis or osteoarthritis, you might struggle with manual dexterity. This can make cleaning your implants harder. Your dental team may recommend more frequent maintenance visits.
Conditions requiring certain medications need careful evaluation. Studies show the dental implant success rate remains similar between older and younger patients when risk factors are properly managed.
Medication and Healing Concerns
Several common medications affect implant surgery and healing. You need to discuss all your medications with your dentist before treatment.
Blood thinners like aspirin, Clopidogrel, or DOACs increase bleeding risk. Your dentist will work with your doctor to determine if you should adjust your medication schedule. Most patients continue their medications without interruption.
Bisphosphonates and denosumab for osteoporosis raise your risk of medication-related osteonecrosis of the jaw (MRONJ). High-risk patients include those on IV infusions for over 5 years or anyone taking these drugs with steroids.
Your healing may take longer than younger patients. Reduced muscle mass affects bite strength and coordination. Beta-blockers can extend how long your mouth stays numb after local anesthesia.
Tell your dentist about all your medications, including over-the-counter drugs and supplements. This helps prevent complications and ensures proper healing.
The Dental Implant Process After Age 60
The dental implant procedure follows specific steps designed to ensure success, starting with a thorough evaluation of your health and bone structure, followed by personalized planning and surgical placement of artificial tooth roots.
Initial Consultation and Candidacy Evaluation
Your first visit to an implant dentist involves a comprehensive examination of your oral health and medical history. The dentist will take X-rays or CT scans to check your jawbone density and quality.
Getting a dental implant in older age requires assessment of any existing medical conditions like diabetes or heart disease.
You’ll discuss current medications with your dental team. Some drugs can affect healing or bone integration. The dentist evaluates your gum health and remaining teeth to identify any issues that need treatment first.
Key factors evaluated include:
- Jawbone density and volume
- Gum tissue health
- Overall medical stability
- Medication interactions
- Existing dental conditions
Your dentist determines if you need additional procedures like bone grafting before implant placement. This consultation helps create a clear picture of your candidacy for dental implants.
Customized Treatment Planning
After your evaluation, your implant dentist develops a personalized treatment plan based on your specific needs. The plan outlines how many implants you need and where they’ll be placed in your jaw.
Your dentist uses imaging technology to map exact placement locations for optimal results.
The treatment timeline gets established during this phase. Dental implant treatment includes healing periods between steps. You’ll learn about costs and payment options available to you.
Your dentist explains the type of restoration you’ll receive, whether a single crown, bridge, or full arch replacement. The plan accounts for any preparatory work needed before dental implant surgery.
Dental Implant Surgery and Placement
The dental implant procedure typically uses local anesthesia to keep you comfortable. Your surgeon makes a small incision in your gum to access the jawbone. The artificial tooth roots are carefully positioned into the bone at precise angles and depths.
Each implant is a small titanium post that acts as a replacement tooth root. After dental implant placement, your gums are stitched closed over or around the implant.
A healing period of several months allows osseointegration, where the implant fuses with your jawbone.
Once healing completes, a second minor procedure attaches an abutment to each implant. The abutment connects the implant to your final restoration.
The treatment process can take several months, but this timeline ensures proper integration and long-term stability.
Types of Dental Implants and Innovative Solutions for Seniors
Several implant types address the specific needs of seniors over 60, from complete tooth replacement to solutions that work when bone loss is severe. Modern options provide stability without always requiring complex bone grafting procedures.
Full Mouth Dental Implants and All-on-4
Full mouth dental implants replace all your upper or lower teeth using multiple implants that support a fixed arch.
The All-on-4 technique uses just four implants positioned at specific angles to hold an entire set of teeth in place.
This approach works well if you have some bone loss because the angled placement uses the strongest areas of your jaw.
You can get a full set of teeth in one day, which means you leave the dental office with functioning teeth rather than waiting months.
The All-on-4 system supports full-arch restorations without bone grafting by engaging denser bone zones. Your new teeth stay fixed and don’t slip when you eat or talk. All-on-6 is similar but uses six implants for added stability if your bone allows it.
Mini Dental Implants and Zygomatic Implants
Mini dental implants are narrower than standard implants and work when your jawbone is too thin for regular-sized implants. They require less invasive surgery and often cost less than traditional implants.
Zygomatic implants anchor into your cheekbone instead of your jawbone. Zygomatic implants are ideal for seniors with advanced upper jaw bone loss and eliminate the need for bone grafting entirely.
These longer implants bypass areas where bone has deteriorated.
Your dentist might recommend zygomatic implants if you’ve worn dentures for many years and your upper jawbone has shrunk significantly.
The procedure is more complex than standard implants but gives you a stable foundation when other options won’t work.
Implant-Supported Dentures and Overdentures
Implant-supported dentures attach to implants placed in your jaw, giving you much better stability than traditional dentures.
You can choose between fixed dentures that stay in permanently or overdentures that snap onto implants but can be removed for cleaning.
Fixed implant-supported dentures work like natural teeth and don’t need to be taken out. Overdentures use two to four implants with special attachments that hold your denture securely but let you remove it at night.
Implant-supported overdentures are recommended when fixed solutions aren’t possible due to bone conditions or budget constraints.
They cost less than full mouth implants but still prevent the slipping and discomfort of regular dentures. You’ll find eating and speaking much easier compared to dentures that rest only on your gums.
Costs and Long-Term Outlook
Dental implants represent a significant financial investment, but understanding the costs and potential lifespan helps you make informed decisions about your oral health after 60.
Cost of Dental Implants for Seniors
The cost of dental implants for seniors typically ranges from $3,000 to $6,000 per tooth. This price includes the implant post, abutment, and crown.
If you need multiple teeth replaced, All-on-4 implants cost between $15,000 and $30,000 per arch. Implant-supported dentures are another option at $6,000 to $20,000 per arch.
Additional costs you might encounter:
- Bone grafting: $500 to $3,000
- Medical clearances: $200 to $500
- CT scans and imaging: $300 to $600
Original Medicare doesn’t cover dental implants in most cases. However, Medicare Advantage plans may offer limited dental benefits.
Average out-of-pocket dental expenses for Medicare beneficiaries exceed $800 annually, with one in five spending over $1,000.
Many dental practices offer senior discounts of 5% to 20%. AARP members may qualify for additional savings at participating offices.
Implant Longevity and Success Rates
Dental implants have high success rates across all age groups. For those aged 65 to 74, success rates reach 96% to 98%. Even patients 85 and older see success rates of 92% to 95%.
With proper care, your implants can last 20 years or longer. Many patients keep their implants for life. This makes them more cost-effective long-term compared to dentures that need replacement every 5 to 7 years.
Factors that affect how long your implants last:
- Daily brushing and flossing
- Regular dental checkups every six months
- Not smoking
- Managing conditions like diabetes
- Maintaining good bone density
Your overall health matters more than your age when it comes to implant success. Even patients in their 90s have received implants successfully.
Caring for Dental Implants as You Age
Proper care becomes increasingly important after 60 as your body’s healing capacity changes and conditions like reduced manual dexterity can affect your ability to maintain oral hygiene.
Understanding recovery expectations and adapting your cleaning routine helps protect against implant failure.
Post-Surgery Recovery and Healing
Your body takes longer to heal after 60, which affects osseointegration—the process where your jawbone fuses with the implant. This bone integration typically takes three to six months, though it may extend longer in older adults.
You’ll need to follow your dentist’s post-surgery instructions carefully. This usually means eating soft foods for several weeks and avoiding the surgical site when brushing.
Watch for signs of complications like excessive swelling, persistent pain beyond the first week, or bleeding that doesn’t stop within 24 hours.
Your bone density plays a major role in healing success. If you have conditions like osteoporosis or take certain medications, discuss these with your dentist before surgery.
They may recommend additional healing time or specific supplements to support bone health during recovery.
Maintenance and Oral Hygiene Tips
Conditions like arthritis can affect your hand strength and dexterity, making standard brushing difficult. Consider using an electric toothbrush with a larger grip or adaptive handles that are easier to hold.
Clean around your implants twice daily using these tools:
- Soft-bristled toothbrush or electric toothbrush
- Interdental brushes to clean between implants
- Water flosser for hard-to-reach areas
- Non-abrasive toothpaste
Schedule professional teeth cleanings every three to six months. Your dentist will check for peri-implantitis, an infection that can lead to implant failure if left untreated.
If you struggle with daily cleaning due to physical limitations, you may need more frequent appointments to maintain proper plaque control.
Frequently Asked Questions
Bone quality plays a major role in implant stability, but age itself does not disqualify older adults from treatment. Most seniors heal predictably when their overall health is stable, and proper maintenance ensures long-term success.
How does bone density affect dental implant success as we age?
Your bone density directly impacts how well an implant anchors in your jaw. As you age, your jawbone can become less dense, especially if you’ve had missing teeth for several years.
Lower bone density doesn’t automatically mean you can’t get implants. Special implant designs work well even in softer bone. For example, NDI implants are preferred for their high primary stability in softer bone, which is common among older patients.
Your dentist will evaluate your bone quality using 3D imaging before recommending specific implant types. Some implants are designed with features that help them grip softer bone more effectively.
Are dental implants a viable option for individuals over 60 with missing teeth?
Yes, dental implants remain a reliable option for people over 60. Your overall health matters more than your age when determining if you’re a good candidate.
Implants work by replacing your tooth root, not just the visible part of your tooth. This helps preserve your jawbone and prevents the sunken facial appearance that often comes with tooth loss.
Many seniors receive implants successfully. Your dentist will check factors like gum health, bone structure, and medical conditions to create a treatment plan that fits your specific needs.
What are the healing time considerations for dental implants in older adults?
Your healing time depends more on your overall health than your age. Seniors with stable health conditions typically heal just as well as younger patients.
The implant needs time to bond with your jawbone through a natural process. This usually takes several months, though the exact timeline varies based on your bone quality and the implant location.
Your circulation and bone metabolism affect healing speed. If you have well-controlled health conditions and good nutrition, your body can support the healing process effectively.
Your dentist will monitor your progress and let you know when the implant is ready to support your new tooth.
Can dental implants improve a senior’s quality of life and how?
Dental implants can significantly improve your daily life by restoring your ability to eat comfortably. Unlike dentures that can slip or cause sore spots, implants stay fixed in place.
You’ll be able to speak more clearly without worrying about loose teeth. Many seniors find they can enjoy foods they had to avoid with dentures, which helps improve their nutrition.
Implants also help maintain your facial structure by preventing bone loss in your jaw. This keeps your face from looking sunken and can boost your confidence in social situations.
What special care do dental implants require in the context of senior oral health?
Your implants need regular brushing and flossing just like natural teeth. The good news is that fixed implants are easier to clean than removable dentures.
You should brush twice daily and floss around your implants to prevent gum inflammation. Special floss threaders or water flossers can make cleaning easier if you have arthritis or limited hand mobility.
Pay attention to your gum health around the implants. Healthy gums help protect the bone that supports your implants. If you notice any bleeding, swelling, or discomfort, contact your dentist right away.
How often should seniors follow up with their dentist after getting dental implants?
You’ll need more frequent visits right after your implant surgery. Your dentist will want to check healing progress at specific intervals during the first few months.
Once your implants are fully healed and functioning, regular checkups every six months are typically sufficient.
These visits allow your dentist to examine the implants, clean around them professionally, and catch any potential issues early.
If you have certain health conditions like diabetes, your dentist might recommend more frequent monitoring. Always attend your scheduled appointments, as they help ensure your implants last for many years.